COVID-19 field hospital to be finished by Friday
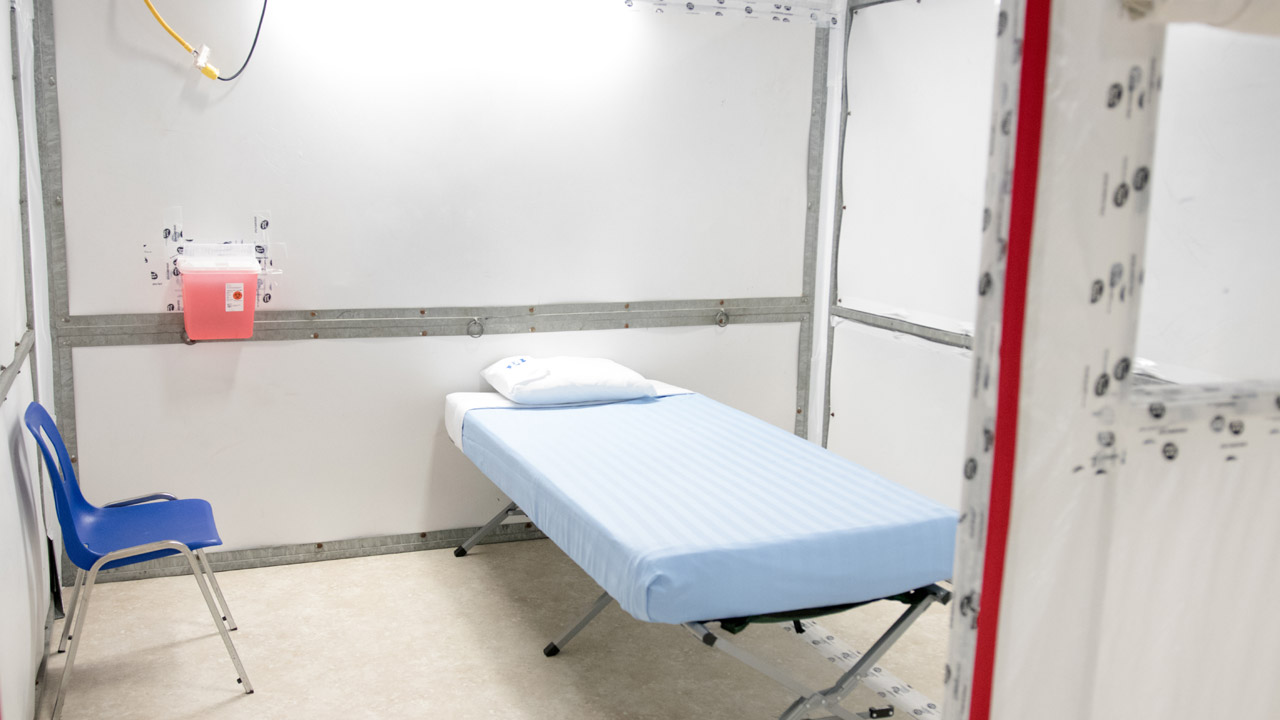 CREDIT: ANGELA MCINNES
CREDIT: ANGELA MCINNESA temporary field hospital at the Western Fair Agriplex will be put to use if the London Health Sciences Centre needs extra space for recovering COVID-19 patients.
A temporary field hospital for recovering London and area COVID-19 patients is expected to be completed by Friday.
The hospital, located at the Western Fair District Agriplex on Florence Street, is managed by the London Health Sciences Centre (LHSC). It is being prepared for readiness but will only be used if necessary.
“The success for this facility is that we build it, we get it ready, and we never use it,” Neil Johnson, LHSC CEO and president, told the media during a tour on Tuesday. “But that success point is not something that we can control. That’s really up to what the virus is doing and what our community is doing in terms of social isolation.”
Work on the hospital began April 3, taking a team of 50 to 60 workers in 16-hour shifts. Once ready, the Agriplex will house 144 total beds intended to give recovering COVID-19 patients a place to recuperate off-site of the LHSC, freeing up more space at the main hospital for those in critical condition.
There will be room to expand to 500 beds should future need arise. These additional beds would be in a separate section of the facility and could expand to include other patient groups as determined by the LHSC’s pandemic response.
The field hospital will be equipped to provide care for patients with low immunity and low needs who require basic restorative care. There is a chance that some of those patients will need palliative care as well.
Divided into pods of 18 beds, the rooms have been staggered to offer privacy to patients. In accordance to hospital policies, there will be no visitation allowed, although the LHSC is looking into potential virtual visitation.
The partitions, observation windows and floors are constructed of flexible plastic materials designed for cleanability. The hospital will include oxygen suppliers, medical IVs, and chest X-ray machines to support respiratory issues. There will not be any ventilators needed for patients who are at the recovery level.
“When [patients] are finished being critically ill, we wean them from the ventilator so that they're breathing on their own, and then typically they would have a face mask or a high concentration of oxygen, and then gradually as their lungs improve and the rest of their condition improves, we would wean down the amount of oxygen, and put them in ward beds outside of the ICU,” said Ian Ball, a critical care physician with the LHSC. “Then there would be a recovery phase where some of them may be so weak that they would have to learn to walk again and do their activities and daily living.”
Ball said it is possible that patients in the intensive care unit (ICU) could need ventilation for weeks. However, he was unable to estimate how long a recovery phase could last.
“The Italians just published yesterday in the Journal of the American Medical Association that a lot of their patients in the original wave are still in the ICU and still on ventilators, so the recovery is probably quite long compared to a lot of the illnesses that we're used to treat in the intensive care units,” he said.
LHSC representatives at the tour said that putting the hospital together was a significant collaborative effort between multiple partners including the City of London and the Western Fair District, as well as suppliers and food services.
If the location is put into operation, medical teams will be made up of roughly one physician, two nurses, and a personal support worker for approximately six patients in eight-hour shifts, rotated 24-hours a day.
As of April 8, the LHSC is treating a total of 26 patients for COVID-19, with eight in critical care and 18 in other inpatient units. In a best-case scenario, the field hospital will never be put to use.
'We put the players on the field and then see what COVID does. We need to be ready to respond,' Ball said. “Our CEO's directive is that we need to be ready. By the time you know that you're going to need it, it's a bit late to start setting it up. As quick as this has been to set up, we need to be ahead of this and be ready to go if we need it.”

















